- Your skin
-
Our products
Do you know well atopic dermatitis ?
DEXERYL supports you and take care of your dry skin each day
-
CLINICAL RESULTS
- About dexeryl
Effective strategies for treating eczema on arms and elbows, with particular attention to fold care. Practical tips for symptom management and improving skin health
Summary
Eczema is a common inflammatory skin condition characterized by dry skin, itching, and typical eczema symptoms (red patches, blisters, oozing, and crusts). Eczema on the arms can occur at any age and affects the flexural folds, elbows, and wrists.
Eczema on the arms and elbows often appears during atopic dermatitis but can also emerge from contact dermatitis.

Eczema on the arms and elbows may be related to genetic factors, especially in cases of atopic dermatitis, where a family predisposition to allergies and atopic diseases is common. This results in dysfunctions of the skin barrier, making it permeable to allergens and irritants. The immune system then overreacts in an allergic manner, producing the signs of arm eczema.
Environmental factors like airborne allergens (pollens, dust mites, animal dander) and pollutants, chemical irritants, climate conditions, unsuitable hygiene habits, or specific food allergens can trigger or exacerbate eczema in the folds of the arms and elbows.

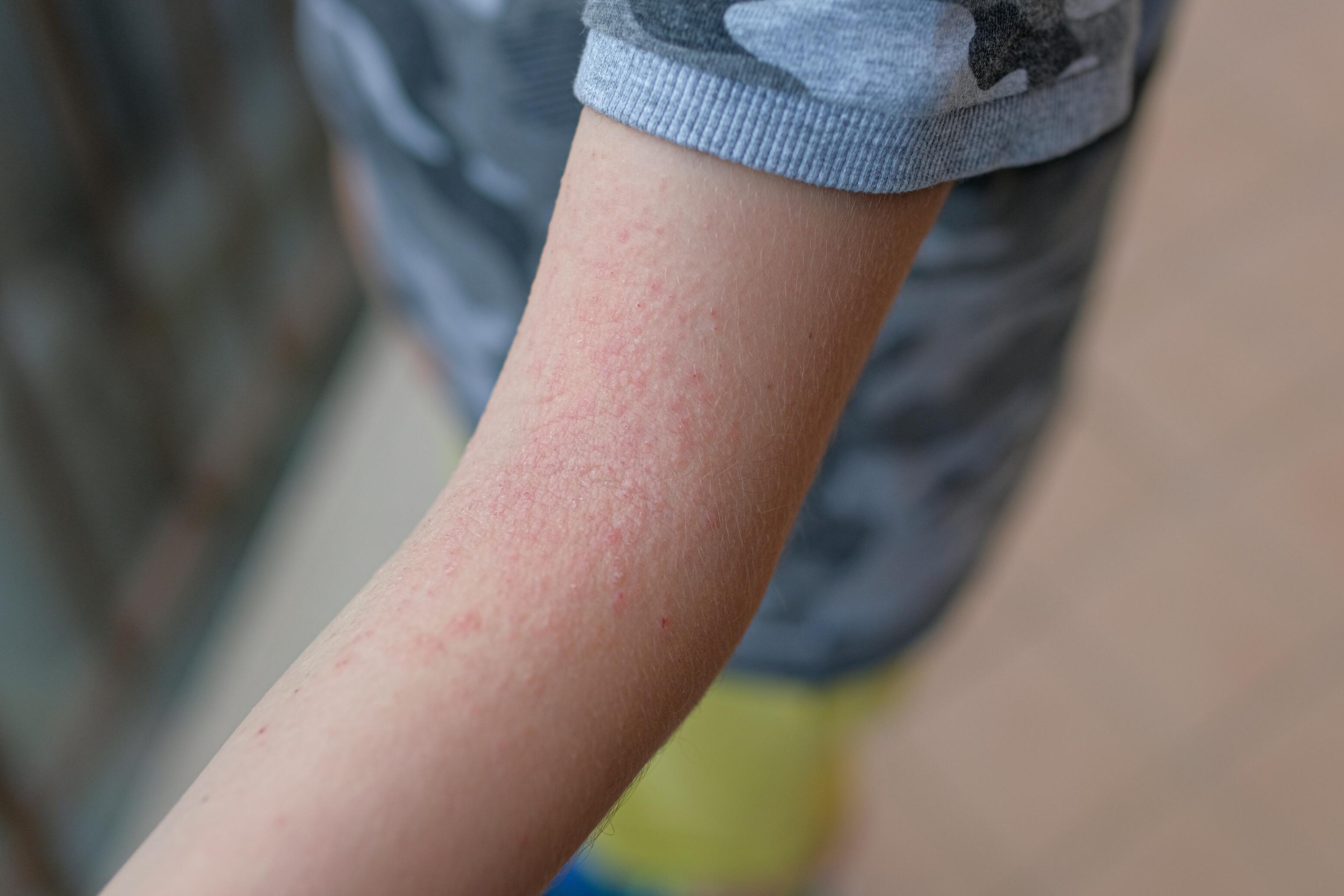
Atopic dermatitis, the most prevalent variant of eczema, commonly initiates during childhood. It is distinguished by its hallmark features: skin dryness, persistent itching, and notable skin lesions, all unfolding in a pattern characterized by periodic exacerbations.
Though less common than on the hands, contact eczema can occur on the arms. Caused by a reaction to an allergen or irritant in direct contact with the skin, contact eczema presents as a rash directly on the exposed area. It is commonplace on the wrists where bracelet materials can provoke various allergies (leather, nickel, chrome, adhesives).

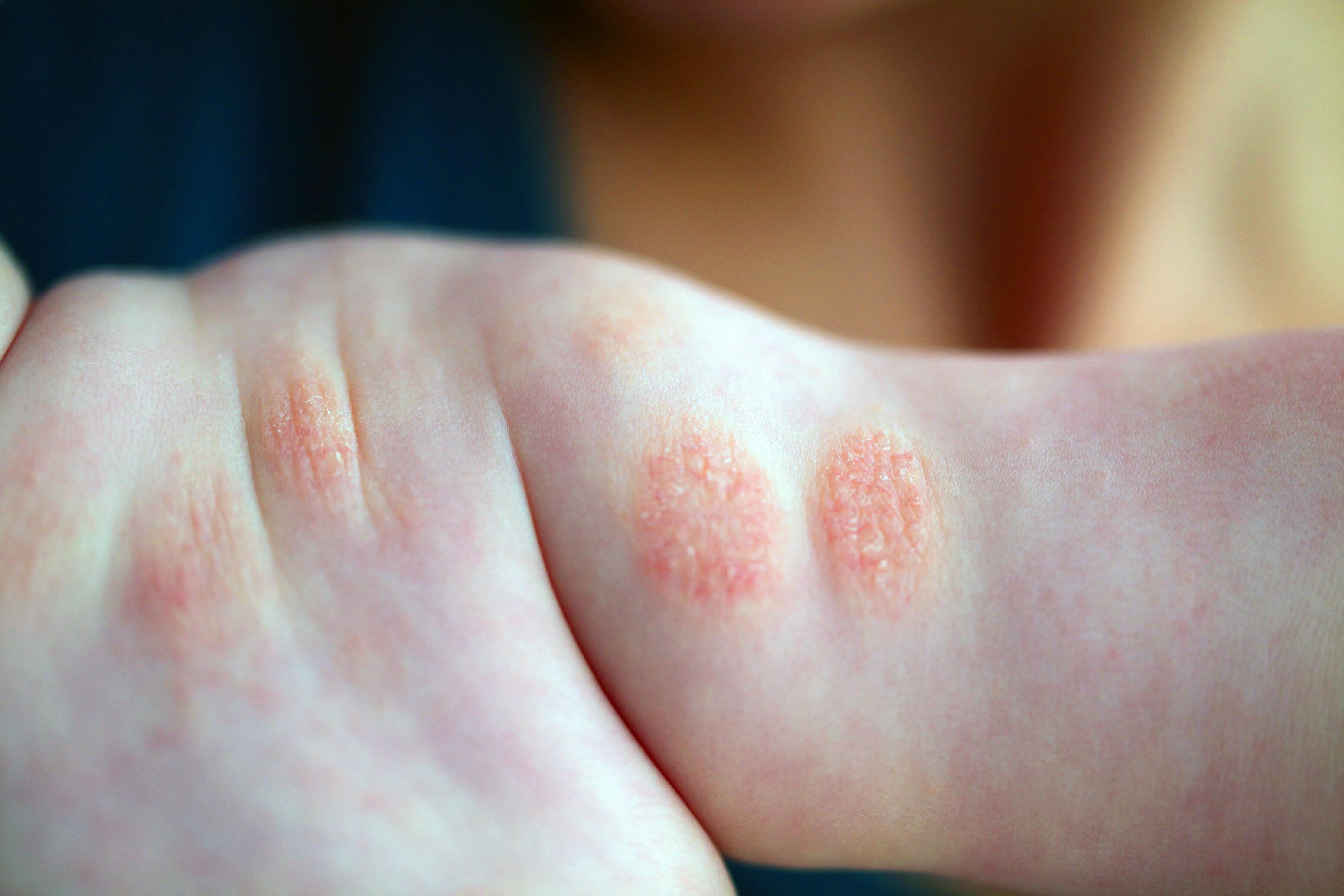
Nummular eczema frequently affects the arms and elbows. It appears as well-defined round patches. Its exact causes are still poorly understood, but several triggering factors, such as injuries and infections, have been identified.
The doctor inquires about any family history of allergic diseases, atopic dermatitis, and exposure to potential allergens or irritants. Lifestyle and environmental factors are reviewed to identify home and workplace aggravating factors.
Then, the doctor examines the appearance, location, and characteristics of the skin lesions. The distribution of eczema in the folds and on the rest of the body provides essential clues.
Allergological tests, such as patch tests, can be carried out to identify a contact allergy.
Other tests may be necessary in specific cases, such as measuring IgE levels in the blood, searching for skin infections, or skin biopsies.
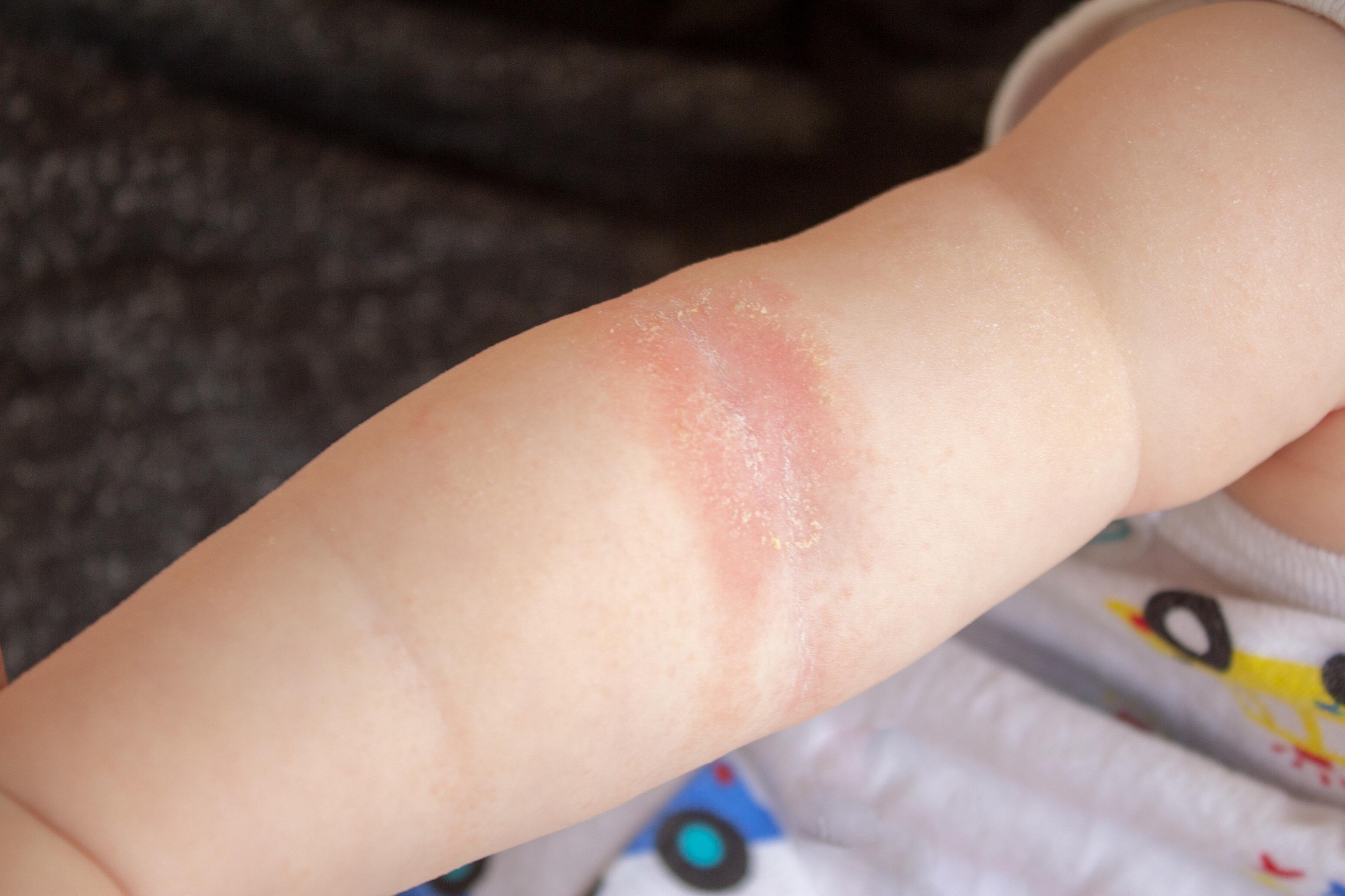
In infants, the signs of eczema typically appear on the extensor surfaces (outer sides) of the arms and elbows. Atopic eczema also affects the face, neck folds, scalp, and legs.
The lesions are characterized by redness, blisters, oozing, and crusts. They can cause discomfort and sleep disturbances.
As children grow, the symptoms of eczema move to the inner folds of the arms, elbows, and wrists. They also affect the knees, ankles, and neck.
The eczema becomes drier and less exudative. Some skin areas thicken (lichenification), taking on a whitish, scaly appearance. Scratch lesions and superinfections are common.

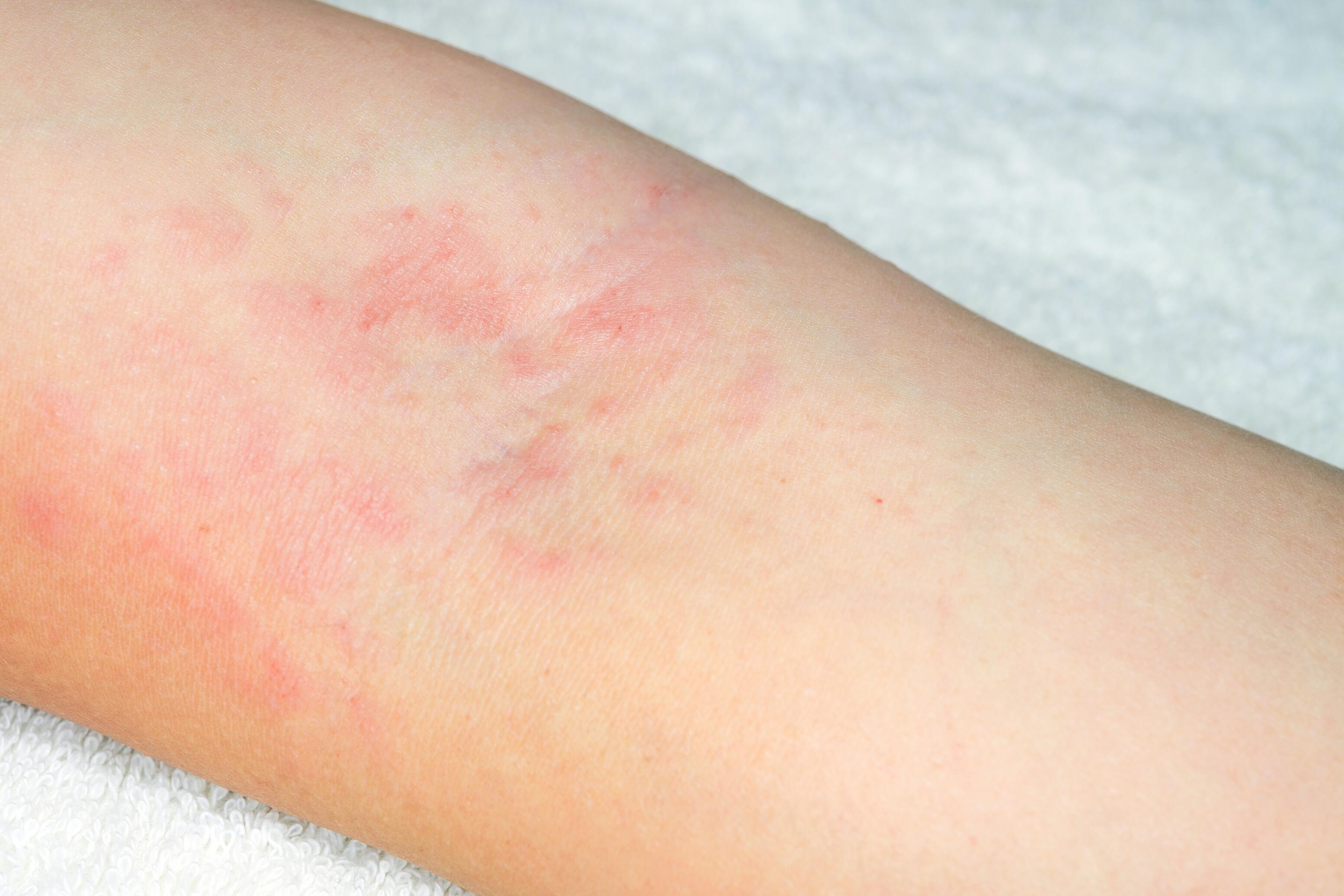
Eczema on the arms in adults mainly affects the flexural folds and elbows. Lesions are also found on the hands, the popliteal fossae (behind the knees), and the face.
The skin can be extremely dry with chronic lichenified lesions due to scratching and an increased risk of cracks and skin superinfections. The chronic nature of the disease can significantly impact the quality of life, sleep, and mental health.
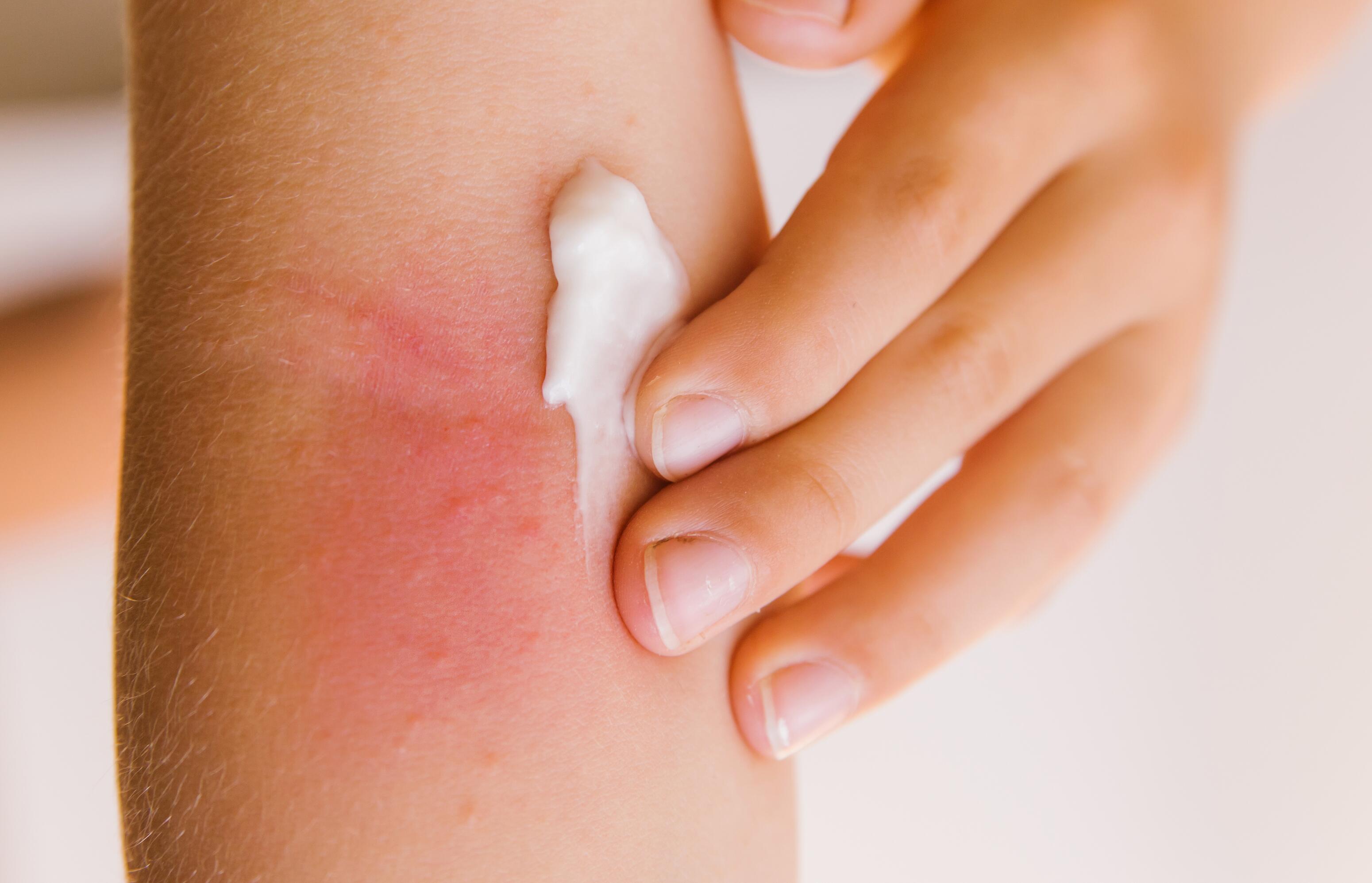
Daily skin hydration with emollients restores the skin barrier and reduces dryness, itching, and flaking. They should be applied all over the body twice daily.
Topical corticosteroids are the first treatment for eczema flares. They reduce inflammation and itching.
In cases where topical corticosteroids are contraindicated, doctors may prescribe topical calcineurin inhibitors (such as tacrolimus).
These treatments are indicated for severe eczema flares that are resistant to topical treatments. These include phototherapy, Janus kinase inhibitors, cyclosporine, and monoclonal antibodies.
Here are some tips for eczema prevention and daily skin care:
Apply emollient creams twice a day, especially after showering or bathing when your skin is still slightly damp, and increase skin hydration in winter, mainly if the weather is cold and dry. Opt for emollients with a simple formula, allergen-free and rich in lipids.
Stress is a common trigger factor for eczema in adults. To prevent it, engage in relaxation activities (meditation, yoga, sophrology).
References:
1. Nemeth V, Evans J. Eczema. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2023 Jan. [Disponible sur :] https://www.ncbi.nlm.nih.gov/books/NBK538209/
2. Kolb L, Ferrer-Bruker SJ. Atopic Dermatitis. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2023 Jan. [Disponible sur :] https://www.ncbi.nlm.nih.gov/books/NBK448071/
3. Litchman G, Nair PA, Atwater AR, et al. Contact Dermatitis. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2023 Jan. [Disponible sur :] https://www.ncbi.nlm.nih.gov/books/NBK459230/
4. Robinson CA, Love LW, Farci F. Nummular Dermatitis. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2023 Jan; 2022 Oct. [Disponible sur :] https://www.ncbi.nlm.nih.gov/books/NBK565878/
5. Lyons JJ, Milner JD, Stone KD. Atopic dermatitis in children: clinical features, pathophysiology, and treatment. Immunol Allergy Clin North Am. 2015 Feb;35(1):161-83.
6. Wollenberg A and al. European guideline (EuroGuiDerm) on atopic eczema - part II: non-systemic treatments and treatment recommendations for special AE patient populations. J Eur Acad Dermatol Venereol. 2022 Nov;36(11):1904-1926.